Acute otitis media (AOM) is an acute inflammation of the middle ear. It is very common in early childhood with a peak prevalence between 6 and 18 months of age. Causes may be multifactorial, often secondary to the Eustachian Tube dysfunction during a viral upper respiratory infection.
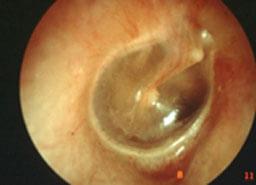
Normal Eardrum
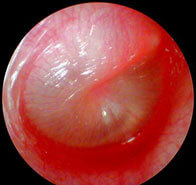
Acute Otitis media
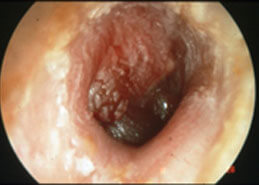
Post AOM infection week 1
Diagnosis
- Acute onset of ear pain, irritability, fever, anorexia, vomiting or lethargy
- Inflamed bulging tympanic membrane (TM) with a middle ear effusion
Febrile, crying children may have a red TM. In addition, look for:
- Loss of normal TM landmarks and light reflex
- Bulging TM with a doughnut or bagel shaped appearance
- Middle ear effusion, possible signs include an air fluid level, reduced TM mobility on otoscopy or otorrhoea due to TM perforation
In febrile infants < 6months the diagnosis of AOM may be difficult to confirm and other more serious causes should also be considered.
The middle ear effusion may take up to 12 weeks to resolve after AOM and is not diagnostic of AOM in the absence of acute symptoms or TM inflammation.
Management
Analgesia
Symptomatic treatment with a regular analgesia, ibuprofen and/or paracetamol is recommended.
Antihistamines, decongestants and corticosteroids are not effective in AOM.
Antibiotic therapy versus observation
Bacterial resistance is an increasing public health challenge. Although in majority of cases of AOM bacteria are isolated from the middle ear fluid, most children improve with analgesia alone within 48 hours.
Antibiotics are indicated in children < 2 years of age with AOM particularly if they have bilateral or severe AOM (severe otalgia, systemically unwell, temperature >39 degrees). These children are often treated with antibiotics for 10 days.
In children > 2 years of age, the current recommendation is observation initially, starting antibiotics if there is no is no improvement after 48 hours. However, if symptoms are severe, antibiotics can be considered immediately.
Choice of antibiotics
High dose amoxicillin is the first choice (90 mg/kg per day in 2 divided doses).
In those who have a penicillin allergy, oral cephalosporin’s such as cefaclor and cefuroxime are effective options.
Children who have taken amoxicillin in the past 30 days, who have purulent conjunctivitis or a history of AOM unresponsive to amoxicillin, should be treated with high dose amoxicillin/clavulanate (Augmentin).
If symptoms fail to improve after 72 hours of antibiotic therapy then high dose amoxicillin/clavulanate or intramuscular ceftriaxone is recommended.
Complications
Otitis media with effusion (OME) is common after AOM. The majority resolve spontaneously. Persistent OME beyond 3 months warrants ENT referral.
Recurrent AOM may warrant surgical intervention. The current recommendation is if children have ≥3 episodes in 6 months, or 4 episodes within 12 months with at least 1 episode during the preceding 6 months, an ENT opinion may be appropriate.
TM perforation is common in AOM, causing otorrhoea and often relief of pain. It does not alter AOM management.
Acute mastoiditis is a rare complication of AOM and may be associated with intracranial complications. Diagnosis is based on post auricular inflammation, a protruding auricle and AOM. This requires prompt ENT referral.
Key points
- Diagnosis of AOM requires acute onset of symptoms, middle ear inflammation and effusion
- Routine antibiotic therapy is not warranted in non-severe AOM
- Prompt specialist consultation is recommended for neonates with suspected AOM, children who are systemically unwell, have a cochlear implant or mastoiditis
- ENT referral is warranted for recurrent AOM and persistent OME beyond 3 months